Skin
Psoriasis
Psoriasis is a chronic skin disease with a high degree of morbidity and comorbidity, such as cardiovascular and psychiatric conditions. A strong genetic basis for psoriasis is well established, and we have seen remarkable advances in the genetic and mechanistic understanding of the disease. However, we still hold large gaps in our knowledge and management, and novel integration of large-scale data and technologies are predicted to play important roles to increase our understanding.
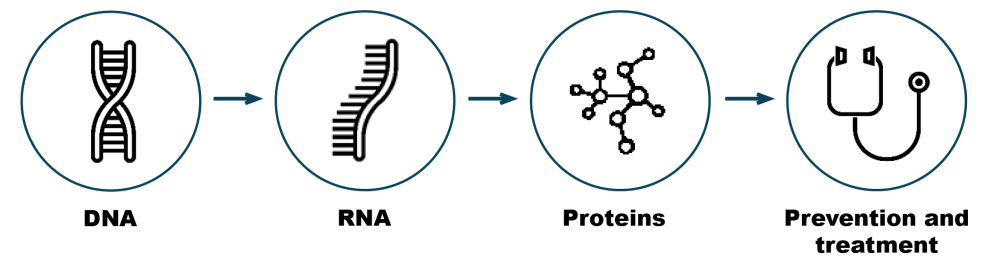
From gene sequencing to clinical use
In our project we will use a multi-layered approach that integrate genetic, transcriptomic and proteomic data with the aim to better understand the biology of psoriasis. We are utilizing available genotype data from three large population-based cohorts (HUNT, Tromsø and UK Biobank), and are linking these to regional- and national health registries to obtain high precision psoriasis phenotypes. In addition, we are studying both global and single-cell gene expression and protein levels from samples in our psoriasis biobank.
We are working at the K.G. Jebsen Center for Genetic Epidemiology. Laboratory experiments and analysis are performed in close collaboration with established infrastructures at St. Olavs hospital and NTNU, in collaboration with our colleagues at University of Michigan. Our effort aims to reveal novel mechanisms and drug targets for psoriasis.
Psoriasis is a common disease
Psoriasis is a chronic immune-mediated skin disease with an estimated global prevalence of 1-3% [1]. The rate of psoriasis differs among nations, and people of European descent are at increased risk. In Norway, the prevalence is amongst the world’s highest, with estimates ranging from 5.8% in the HUNT Study [2] to 11.4% in the Tromsø Study [3]. The incidence seems to be increasing over time. Psoriasis affects women and men equally, and the mean age of onset for the common form is in the late twenties.
Psoriasis represents a substantial burden on public health
Psoriasis is associated with a high degree of morbidity, and the disease is known to greatly affect quality of life, including reduced levels of employment and income [4]. Because the disease has a relapsing course, patients with psoriasis usually need lifelong care, which also means a lifetime of expenses for affected individuals and society. Psoriasis has been associated with a spectrum of comorbidities, including psoriasis arthritis, cardiovascular and psychiatric conditions. Suggested links between psoriasis and the comorbidities include shared genetic susceptibility, systemic inflammation and common risk factors. The treatment approaches for psoriasis includes topical and systemic therapies, and we have seen remarkable advances in treatments options over the last decades. However, we still hold large gaps in our knowledge and management of the disease.
Genomic studies have driven major breakthroughs for psoriasis
Psoriasis is a complex disease that is triggered by environmental factors in genetically susceptible individuals. The heritability is estimated at 60% to 90%, with an area (locus) on chromosome 6p (HLA-Cw6 in PSORS1) as the strongest known genetic risk factor [5]. Assisted by the recent development of large-scale high-throughput genomics, more than 60 genetic loci have been linked to psoriasis [6, 7]. Using these results, genetics support the role of a dysregulated immune system through pathways that involves cells of both adapted and acquired immunity. Despite providing remarkable insight into disease pathogenesis, less than 30% of the variance in liability has been accounted for [6], hence a substantial proportion of the genetic risk for psoriasis is yet to be identified.
The Psoriasis Biobank
The carefully built biomedical research infrastructure in Norway provides unique advantages and makes it possible to do extensive multi-omics profiling of psoriasis by utilizing large prospective population studies, HUNT Biobank, high-quality disease-specific registries and tissue from our psoriasis biobank.
References: 1. Parisi, R., et al., Global epidemiology of psoriasis: a systematic review of incidence and prevalence. J Invest Dermatol, 2013. 133(2): p. 377-85. 2. Modalsli, E.H., et al., Validity of Self-Reported Psoriasis in a General Population: The HUNT Study, Norway. J Invest Dermatol, 2016. 136(1): p. 323-5. 3. Danielsen, K., et al., Is the prevalence of psoriasis increasing? A 30-year follow-up of a population-based cohort. Br J Dermatol, 2013. 168(6): p. 1303-10. 4. Stern, R.S., et al., Psoriasis is common, carries a substantial burden even when not extensive, and is associated with widespread treatment dissatisfaction. J Investig Dermatol Symp Proc, 2004. 9(2): p. 136-9. 5. Trembath, R.C., et al., Identification of a major susceptibility locus on chromosome 6p and evidence for further disease loci revealed by a two stage genome-wide search in psoriasis. Hum Mol Genet, 1997. 6(5): p. 813-20. 6. Tsoi, L.C., et al., Large scale meta-analysis characterizes genetic architecture for common psoriasis associated variants. Nat Commun, 2017. 8: p. 15382. 7. Dand, N., et al., Exome-wide association study reveals novel psoriasis susceptibility locus at TNFSF15 and rare protective alleles in genes contributing to type I IFN signalling. Hum Mol Genet, 2017. 26(21): p. 4301-4313.
Useful links
Psoriasis - A systemic disease (Norwegian blog post)
Gene expression in psoriasis (Norwegian blog post)
High BMI increases chance of psoriasis (Norwegian article)




